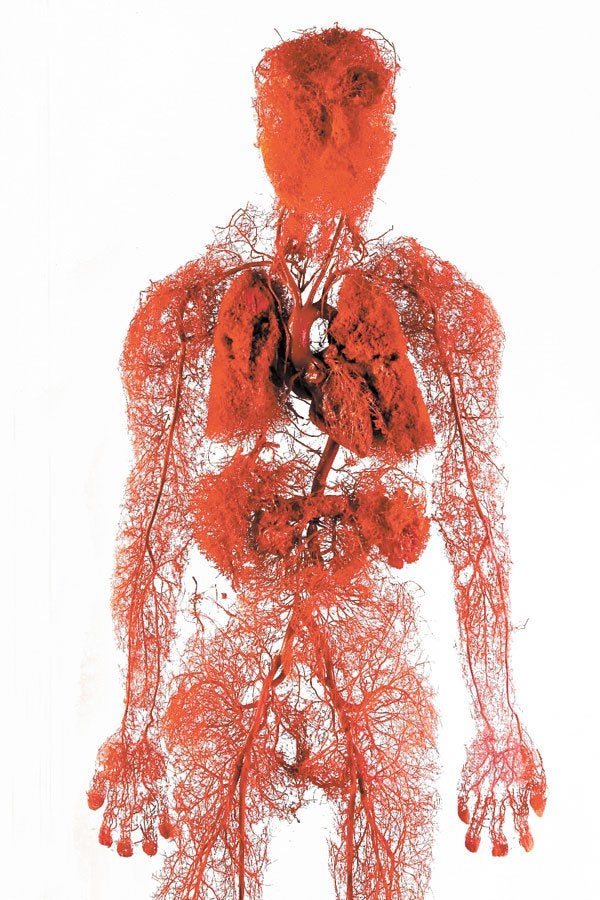
Microvascular tissue is in most human tissues and can be thought of as the foundation of all tissue. Its primary function within the body is to supply nutrients and regulate blood flow.
It is composed of small blood vessels (capillaries, arterioles, and venules) and extracellular matrix that improve microcirculatory blood flow.7,8
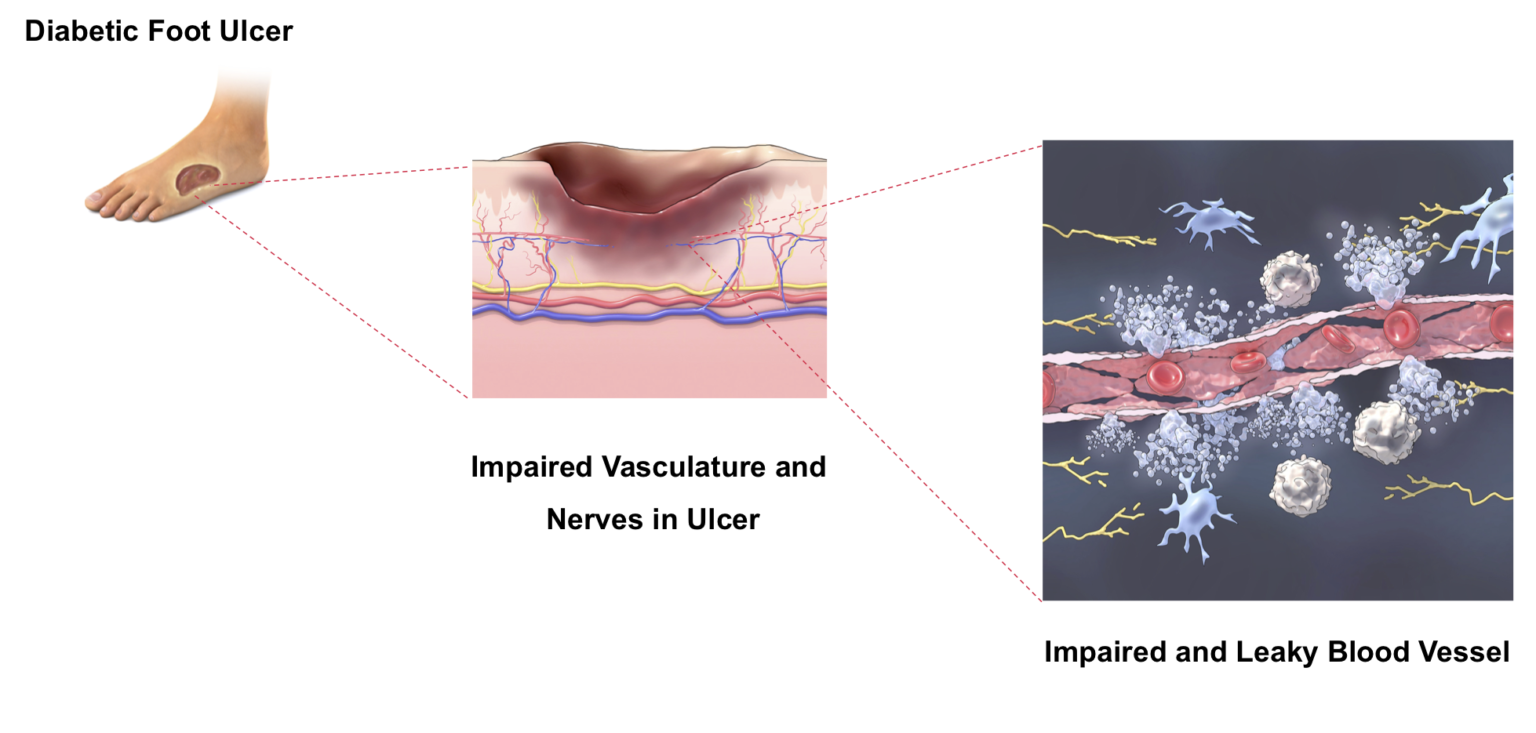
Nonhealing diabetic foot ulcers (DFUs) are stalled wounds with compromised repair capabilities. Less than one quarter of these ulcers will heal with standard wound care after 12 weeks.1
The large clinical and economic burden of nonhealing DFUs continues to escalate, and includes multiple admissions, treatment for infection, neuropathy, and amputations. Up to 34% of the 34 million diabetics in the US will develop a DFU during their lifetime. 2,3 Despite use of advanced therapeutics, the 5-year mortality after amputation from a diabetic foot ulcer is over 45%.4
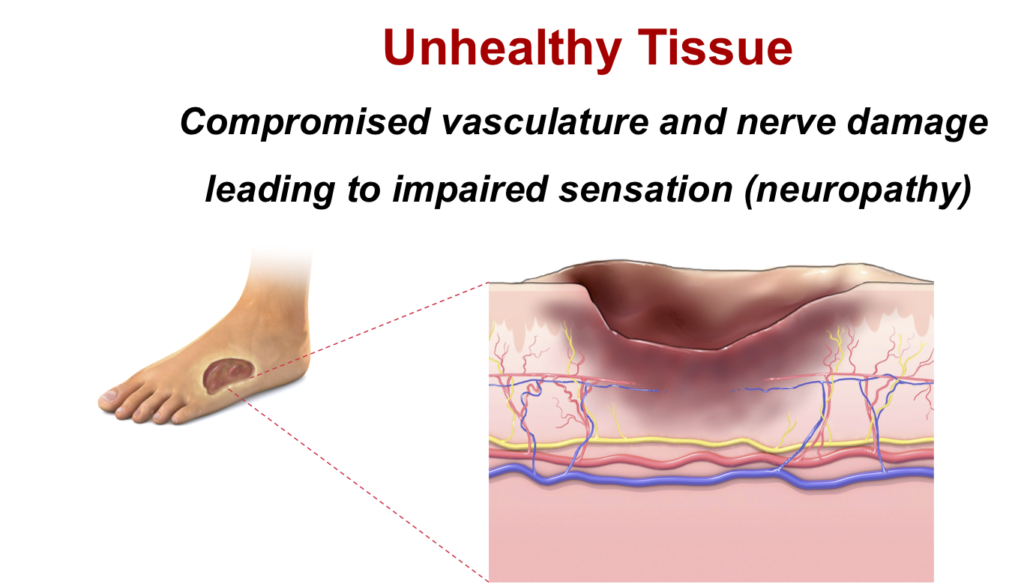
In addition to addressing the compromised vasculature contributing to a nonhealing DFU, microvascular tissue also has the potential to impact the loss of sensation common in diabetes. Leaky capillary walls in diabetic tissue decrease blood flow to the surrounding microvascular tissues, resulting in structural changes that also damage the nerves, and ultimately leading to neuropathy associated with the occurrence and recurrence of DFUs. 5,6
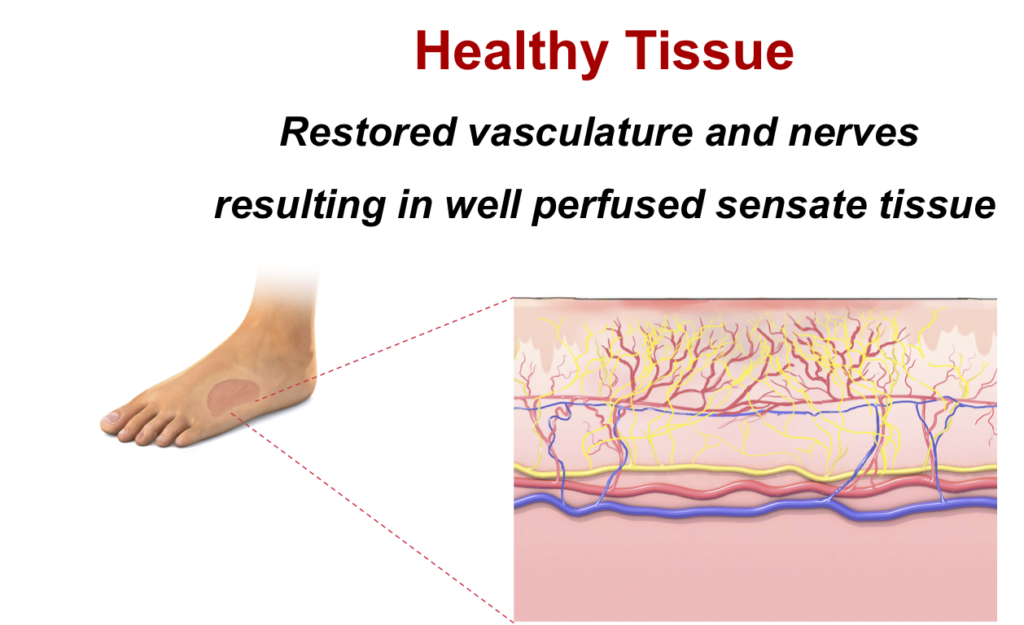
A functioning microvasculature is crucial for closing nonhealing wounds and restoring an environment that translates into well-perfused, sensate, high quality tissue.
2Armstrong DG, et al. N Engl J Med. 376:24 (June 2017). (up to 34% of 34M)
3National Diabetes Statistics Report, 2020. (up to 34% of 34M)
4Armstrong DG, et al. J Foot Ankle Res. 13:16 (2020). (5y mortality <45%)
5Thrainsdottir S, et al. Diabetes. 52:2615 (2003). (vascular changes lead to neuropathy)
6Lavery L, et al. Arch. Intern. Med. 158:157 (1998). (neuropathy predictor of DFU)
7Yuan, S et al. Regulation of Endothelial Barrier Function. Chapter 2: Structure and Function of Exchange Microvessels. Morgan & Claypool Life Sciences. 2010. San Rafael, CA
8Xu, J et al. Vascular wall extracellular matrix proteins and vascular diseases. Biochim Biophys Acta. 2014;1842:2106–2119

©Copyright 2023 MicroVascular Tissues, Inc.